Fluid Therapy 2019: Crystalloid vs. Colloid Therapy
by Dr. Philip R Judge BVSc MVS PG Cert Vet Stud MACVSc (VECC; Medicine of Dogs)
Introduction
Provision of intravenous fluid therapy is one of the most common interventions in veterinary medicine, and is widely used in emergency patients, patients undergoing anaesthesia +/- surgery, and in critical care patients. Fluid therapy is broadly used to manage acute hypovolaemia, to pre-emptively optimise blood flow to tissues in intra-operative patients, and to maintain euvolaemia in patients with critical illness and sepsis – with the ultimate goal in all of these situations to improve tissue oxygen delivery.
From the outset of this discussion, it should be stated that intravenous fluid therapy administration should be viewed in the same context as any other drug administration to patients, because fluid therapy requirements are context-specific – with requirements in acute hypovolaemic shock being different from those required for replacement of fluid losses from wounds, for example, and from those in patients with severe illness and septic shock.
Numerous questions on the efficacy and safety of fluid therapy, in terms of the type of fluid, and the dose of fluid administered to a patient are at present unresolved. In particular, the role, safety and efficacy of synthetic colloids in patients requiring intravenous fluid therapy remains a topic of great interest. This discussion aims to highlight, and clarify some of the current controversies in the crystalloid versus colloid use in fluid resuscitation, as well as to address some of the safety concerns regarding the use of synthetic colloids in septic patients.
Fluid Types
The Starch Fluids (Hydroxy-Ethyl Starch; HES)
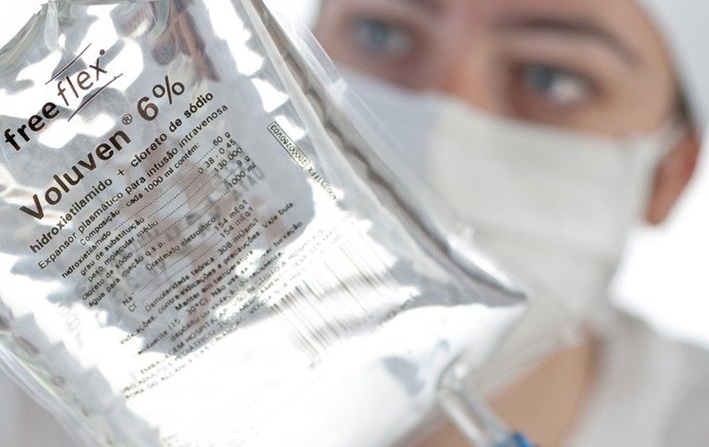
HES is a semi-synthetic colloid fluid therapy suspended as an isotonic solution in either lactated Ringer’s solution or 0.9% saline. HES is derived when amylopectin in potato or waxy maize is modified by the substitution of hydroxyl groups with hydroxyethyl residues on the glucose subunits.
Because of their larger molecular size, it is expected that colloid infusions will lead to a greater plasma volume expansion than crystalloid, and this has been observed in both human and animal studies –with administered volumes producing up to 40% greater increase in plasma volume with colloid infusions in healthy patients – translating to a decrease in fluid volume requirement by the patient of up to 40%. However, in septic patients, the increase in plasma volume produced following colloid infusion is much more modest.
The Crystalloids (0.9% saline; Lactated Ringer’s solution; Normosol etc.)
Crystalloid solutions are solutions of electrolytes in sterile water, and are classified as being balanced or unbalanced, and buffered or unbuffered, according to their composition. Lactated Ringer’s solution and Normosol R are termed balanced and buffered solutions – and contain electrolytes in similar concentrations to those found in normal extracellular fluid. They are also buffered to achieve a pH range closer to mammalian physiological pH than 0.9% saline. They are therefore considered reasonably safe intravenous fluids to use for acute volume resuscitation in most disease states. 0.9% saline is an unbalanced and unbuffered solution that contains sodium and chloride in equal concentrations, with chloride levels approximately 60 mEq/L higher than in normal patients. It also is more acidic than buffered crystalloid solutions (average pH 5.1).
Because crystalloid solutions are simple electrolyte solutions, they will eventually distribute throughout the extracellular fluid space following intravenous infusion. It is expected than up to 75% of an intravenous bolus of crystalloid solution will redistribute to the interstitial fluid space within 30-60 minutes of infusion, leaving 25% within the vascular space for blood volume expansion. This large loss of intravascular fluid is one reason crystalloids are required to be administered in large volumes when treating shock – and was one of the principle reasons colloid solutions have been evaluated as an alternative fluid for resuscitation for many years.
The Crystalloid versus Colloid Debate: The Origins
The debate regarding the risks and benefits of colloid and crystalloid solutions reached a climax in modern-day medicine in 1998, when a review found that the use of human albumin was associated with one additional death for every 17 patients treated. Despite the review having errors in methodology, the review findings were released by secular media. Public awareness of potential concerns with albumin infusion ensued, with interest in the patterns of clinical use of crystalloid and colloid solutions within the medical profession increasing also.
In 2012, two landmark research papers cast doubt over the safety of synthetic colloids in critically-ill patients – citing an increased risk of kidney damage with colloid use. The citing studies were the Scandinavian Starch for severe Sepsis/Septic Shock (6S) trial and the Crystalloid versus Hydroxy-ethyl starch trial (CHEST) studies. Widespread publicity of these studies in popular media prompted the EU to ban the use of synthetic colloids in patients with sepsis. On the basis of these studies, in June 2013, the FDA also issued a safety advisory citing increased mortality and risk for severe renal injury in sepsis. Presently, the FDA recommends avoiding HES in patients with preexisting renal dysfunction, monitoring renal function for at least 90 days in all patients receiving HES, and discontinuing HES at the first sign of renal injury or coagulopathy among those undergoing cardiac surgery with cardiopulmonary bypass. Interestingly, in considering their standpoint and recommendations, the FDA announcement also cited a recent review of 6% tetrastarch (HES 130/0.4) among patients undergoing surgery where, in contrast to the ICU findings, the authors concluded that there is no evidence of harm associated with tetrastarch when used intraoperatively or in the immediate postoperative period.
Adding to this, recently, the Colloids Versus Crystalloids for the Resuscitation of the Critically Ill (CRISTAL) trial, an open-label randomized comparison of crystalloids against colloids early during resuscitation, reported a possible benefit for colloids when used during the resuscitation phase for acute hypovolemia – with the colloid patients having reduced mortality, and less days required with vasopressor therapy and mechanical ventilation.
Yet further adding to the controversy of risk versus benefit to the use of synthetic colloids, in 2011, several journal articles demonstrating benefits of the use of HES were retracted after investigations into some widely cited researchers work revealed some studies purporting the benefit of HES were fabricated. This event removed many of studies up to that time, reporting benefits of colloids in hospitalised patients from the literature, and cast the benefit versus safety of colloids into question further.
The Crystalloid versus Colloid Clinical Studies
In addition to the aforementioned studies, several clinical and experimental studies conducted over the past 20 years or so have shown hydroxy-ethyl starch to have the following effects when used in patients for volume resuscitation in both acute hypovolaemic shock, septic shock and in post-operative patients…
- Attenuation of the inflammatory response
- Mitigation of endothelial barrier dysfunction and increased vascular permeability
- Preservation of intestinal barrier function
- Improved microvascular circulation in patients with sepsis
- More rapid haemodynamic stabilisation and reversal of shock
- Improved intestinal wound healing and anastomosis bursting strength in intestinal surgery
- Require less volume to treat shock than crystalloid fluids.
Despite these studies indicating favourable outcomes with colloid infusions, a long-term benefit, including patient survival, has not been consistently shown. As eluded to previously, more recently, several randomised clinical trials have specifically evaluated the effect of colloid vs. crystalloid fluid resuscitation in critically-ill patients – specifically, those with severe illness and sepsis – with outcome objectives being survival, and complication rates from fluid type. A summary of these trials, and key study findings is listed below…
- SAFE Trial: evaluated the use of 4% albumin in 0.9% saline vs. 0.9% saline
- This trial investigated saline versus albumin fluid administration for fluid resuscitation of patients in ICU
- No overall difference in mortality, number of ICU days, need for mechanical ventilation or renal replacement therapy
- Higher mortality in head trauma patients receiving albumin
- CHEST Trial: evaluating 6% hydroxy-ethyl starch in 0.9% saline vs. 0.9% saline
- This trial evaluated the use of Voluven (6% HES 130/0.4 in 0.9% saline) compared to 0.9% saline for acute resuscitation in ICU
- No overall difference in mortality rate
- Faster normalization of cardiovascular indices with HES
- Less fluid required to achieve cardiovascular stability (30% less fluid)
- Lower rate of cardiovascular failure with HES
- Increased requirement for renal replacement therapy with HES (7% vs. 5.8%; P=0.04)
- 6S Trial: evaluating 6% hydroxy-ethyl starch in Ringer’s acetate vs. Ringer’s acetate
- This trial evaluated tetrapsan (6% HES 130/0.42 in Ringer’s acetate) compared to Ringer’s acetate for acute resuscitation in severe sepsis.
- Increase mortality with HES (51% vs. 43%; P=0.03)
- Increased incidence of acute kidney injury (22% vs. 16%; P=0.04 with HES)
- CRISTAL Trial: evaluating crystalloid solutions with colloid solutions and 28 and 90 day mortality
- This trial evaluated patients admitted to ICU with hypovolaemia, trauma or sepsis, managed with either colloids (plasma, gelatins or HES) or crystalloids (0.9% saline or balanced crystalloids
- No difference in mortality at 28 days
- Significant increase in mortality in crystalloid-resuscitated group at 90 days
- No increase in renal replacement therapy with colloid group (interestingly, doses of colloids were 30 ml/kg/day in this study; other studies have used up to 50 ml/kg/day)
- Colloid-treated patients had more rapid weaning from life-support, and more days alive without ventilation and vasopressor support
- Sepsis Occurrence in Acutely Ill Patients
- A large prospective observational study (Sepsis Occurrence in Acutely Ill Patients) found that HES infusion (median dose 10 ml/kg/day) did not increase the risk for AKI
- Fluids after Cardiac Surgery: Colloids versus Crystalloids
- This study compared 10% HES 250/0.45 to isotonic saline in 262 patients who underwent cardiac surgery
- No evidence of nephrotoxicity—no difference in the daily creatinine, development of AKI by RIFLE (risk, injury, failure, loss, and ESRD) criteria during hospital stay (16% in both groups), or need for renal replacement therapy (1% in each group).
- Patients in the saline group received nearly 60% more volume for fluid resuscitation in the intensive care unit (ICU) than did the HES group (887 versus 1397 ml; P<0.0001).
- Far fewer patients receiving HES required catecholamines the morning after surgery compared with those receiving saline (10.9% versus 28.8%; P=0.001).
- CRYSTMAS Study: Evaluated 6% HES 130/0.4 vs. 0.9% Saline in patients with severe sepsis
- This study was conducted on 196 patients with severe sepsis randomly assigned to treatment with HES or saline.
- Less fluid required to reach haemodynamic stability in HES group
- No differences in renal function between groups
- Non-statistically significant trend toward increased use of dialysis in HES group.
Collectively, these data imply an increased risk for harm – particularly the development of acute kidney injury (AKI) – associated with HES solutions when used in patients with severe illness or sepsis, and have lead the European Society of Intensive Care Medicine to recommend against the use of HES in patients with severe sepsis or those at risk for AKI and to further suggest a moratorium on the use of HES except in the context of a clinical trial. In addition, the United States Food and Drug Administration issued a Boxed warning against their use in critically-
ill patients due to the increased risk of AKI and death.
However, the results of these trials deserve further consideration, because the “on-the-surface” results do not tell the full story. One such consideration is the patient selection within each study. For example, in the 6S trial, a large number of study patients were in sepsis, which resulted in patients being less likely to achieve shock reversal with intravenous fluid therapy alone; whereas, in the CHEST trial, which had a more heterogonous patient inclusion criteria, shock was reversed with less total fluid administered in the HES group. When comparing these two studies, these data imply that HES may be more efficacious for shock resolution when compared to crystalloid in non-septic patients. However, if there is delayed administration of fluids or failure to reverse shock with fluid therapy, there may be greater toxicity and harm associated with HES.
It is important to note also, that both CHEST and 6S studies allowed patients with be stabilised haemodynamically with up to 1000 ml colloids before randomization into crystalloid or colloid treatment groups – with over 60% of the crystalloid group in the CHEST study having received colloid resuscitation – meaning that both study groups may have received potential benefits (or potential toxicity) of colloids that were not considered in the author’s conclusions. There was also a standard deviation of almost 7 days from the time of ICU admission until recruitment in CHEST. That these papers referred to the use of HES in their study to treat hypovolaemia and septic shock as “early resuscitation” could be called into question based on these criteria.
Additionally, the colloid fluid type use in the 6S study was HES 130/0.42, whereas the colloid fluid type used in CHEST was HES 130/0.4. There is clinical and experimental evidence that colloids with higher degrees of substitution carry potentially more risk to the patient that those with lower degrees of substitution. Whether this also impacts the results of the 6S study in terms of mortality compared to the CHEST study is not known.
The Effect of Fluid Type on Study Outcome
The Effect of High Chloride Solutions
It is emerging that high chloride solutions such as 0.9% saline are associated with renal vasoconstriction, decreased glomerular filtration rate, and an increased risk of acute kidney injury and a requirement for renal replacement therapy. Furthermore, high chloride solution administration is associated with a higher incidence of electrolyte and acid-base disturbances, a higher requirement for blood transfusions greater interstitial fluid accumulation and a higher rate of post-operative infections when compared to balanced isotonic crystalloid solutions such as PlasmaLyte A or PlasmaLyte 148.
It is well-known that hyperchloraemic solutions, such as 0.9% saline, induce metabolic acidosis. It is also known that both electrolyte and acid-base perturbations can induce inflammation and hemodynamic instability in animal experiments. The precise mechanisms whereby saline contributes to, or exacerbates acute kidney injury (AKI) are not well understood. Animal studies suggest that high chloride concentrations reduce glomerular filtration rate via tubulo-glomerular feedback. Additionally, saline may directly lead to renal injury, as evidenced by urine neutrophil enzyme levels and renal histology. Inflammation (plasma IL-6) is also increased with saline compared with balanced crystalloid. These observations are not encountered when balanced, buffered, polyionic solutions are used for resuscitation.
Collectively, this evidence strongly suggests that the type of crystalloid used for comparison between crystalloids and colloids is at least as important as the type of HES examined, and may influence the results and interpretation of studies, and that the use of 0.9% saline should probably be avoided in patients for resuscitation.
The Effect of Colloid Solutions
As outlined above, there are several experimental and clinical studies that demonstrate improved outcome in patients when given synthetic (and natural) colloids in varying situations from elective surgery to acute trauma. However, in the more recent studies looking at colloids versus crystalloids, the key marker for study outcome has been mortality – for which there appears no consistent significant difference between crystalloids and colloids, however, there is an increased risk of acute kidney injury. It is worthwhile therefore, noting some outcomes of studies not associated with mortality.
Numerous studies, including some mentioned above, show that the use of colloids, including HES during volume resuscitation offers superior efficiency, meaning that effective volume expansion is achieved with smaller volumes. In the SAFE trial, 29% more saline was given in the first 48 hours compared with albumin; and total fluid balance during this time period was 1 L greater with saline (2.56 versus 3.5 L). This is an important consideration in many patients. Evidence from patients with acute lung injury suggests that higher volumes of administered fluids result in longer duration of mechanical ventilation, and observational data from patients with AKI suggest that fluid overload is associated with reduced survival. Evidence suggests colloids have blood volume expansion 1.2-1.4 times greater than with crystalloid infusion alone – thus smaller infusion volumes required with colloid solutions may confer an advantage to the patient.
Additionally, in anaesthesia, goal-directed therapy with HES has been shown to reduce post-operative nausea, provides earlier return to bowel function, reduced time on mechanical ventilation, and shorter hospital stays
Furthermore, in a study of 50 patients undergoing cytoreductive surgery for ovarian cancer, patients who received 6% (isotonic) HES 130/0.4 required less fluid, and less transfusion therapy than patients managed with balanced crystalloids. No difference in urine output, creatinine concentration or urine neutrophil gelatinase-associated lipocalin (renal injury marker) were observed in this study.
Experimental studies in pigs with colonic anastomosis demonstrate increased surgical wound strength and collagen deposition, and improved anastomotic bursting strength in subjects treated with HES over those treated with 0.9% saline, attributed to improved microcirculation and anti-inflammatory effects.
The Difficulties in Interpreting Crystalloid versus Colloid Studies
Fluid Resuscitation End-Points
Fluid resuscitation end-points are currently an area of controversy, with the value of traditional guidelines such as blood pressure restoration and urine output being called into question. This has implications in outcomes of many studies involving crystalloid and colloid fluid therapy – particularly in septic patients, who traditionally respond more poorly to volume resuscitation with intravenous fluids.
The flux in understanding and use of appropriate fluid resuscitation end-points adds to the difficulty of selecting the correct fluid type and dose, and in interpreting studies that use varying resuscitation end-points between and within treatment groups.
As eluded to above, recent data suggest static metrics of resuscitation, such as central venous pressure (CVP), and even arterial blood pressure and urine output, may not accurately correlate with restoration of intravascular volume and improvement in tissue oxygen delivery in the septic patient. Normalising central venous oxygen saturation (> 65%-70%) and rapid serum lactate clearance (> 20% in 2 h) in response to fluid resuscitation (± additional hemodynamic support) have been recommended as more appropriate end-points to fluid therapy resuscitation, and correlate with improved outcome – particularly when combined with measurements of cardiac output, end-tidal carbon dioxide concentration and pulse pressure variation.
Furthermore, critically-ill patients are not homogenous in the severity of their disease, and their responsiveness to fluid loading, and this observation would strongly support the need for individualized resuscitation goals that integrate functional haemodynamic measures, rather than the use of generic resuscitation end-points.
It is important to note, that fluid resuscitation end-points were not standardized in the CHEST or 6S trials – in fact, in many of the large colloid versus crystalloid resuscitation trials – and this introduces an area of potential study error or bias.
Patient Disease
It appears that the patient disease – or context in which synthetic colloids are used, may also play an important role in the relative safety and benefit to the patient.
The risk of using tetrastarch in patients with an intact glycocalyx – such as those with acute trauma, or in healthy patients undergoing anaesthesia for example, may be potentially different to the risks associated in patients with severe sepsis, in which there is significant glycocalyx shedding and disruption. This notion is supported by the CRISTAL trial, which suggested that safety outcomes were improved with HES administration in patients that were responsive to fluid resuscitation (improved cardiovascular parameters, oxygen delivery etc.) over those that were non-responders.
Total Fluid Volume
Excessive fluid administration – regardless of fluid type – appears to have an adverse impact on patient outcome – with the margin of safety with excess fluid administration being perhaps larger in patients with intact glycocalyx. Thus, a patient with intact glycocalyx may tolerate a larger volume of fluid therapy without adverse effects than a patient with sepsis – regardless of the fluid administered. It may, therefore, be more appropriate to administer smaller fluid challenges to septic patients with symptoms indicating hypovolaemia, and to consider earlier administration of vasopressors and/or positive inotropic agents, rather than to manage these patients with large volumes of crystalloid or colloid.
Conclusion:
Despite widespread use in emergency and critical care patients, the science of fluid resuscitation in critical illness requires much-needed research. The recent survival and complication studies comparing colloids with crystalloids have shed new light on this area, and have provided new impetus to evaluate the safety and efficacy of fluid therapy in the critically-ill patient. Additionally, the revised Starling model, and knowledge of the role of glycocalyx in fluid balance have been critical in forcing revision of current fluid therapy practices.
Overall, it appears the context of the clinical situation requiring fluid therapy appears to be crucial when prescribing fluids – and any fluid can be harmful if dosed incorrectly. Optimal dosing of any resuscitation fluid therefore mandates an understanding the dynamic nature of fluid resuscitation, and future investigations will hopefully allow for the development of better tools to guide therapy.
Toxicity of colloids (even with newer lower molecular weight, less substituted HES solutions) and isotonic saline remain a concern in all groups of patients studied to date. Regarding crystalloid fluids, the differences in chloride load and strong ion difference in the various crystalloid solutions also appear to be clinically important.
It appears, at present, that physiologically balanced crystalloids may be the best “default” fluid for acutely ill patients, and that the role of colloids is unclear.
The crystalloid-colloid controversy will undoubtedly continue, and will benefit from further studies, particularly with single-disease patient groups. It is the author’s belief that fluids are drugs and should receive considerable thought in their prescription for patients. It is probable that there is a serious—and late—hazard when starch is used as a resuscitation fluid in the ICU – particularly at doses approaching the manufacturers stated daily dose limit. Whether the use of starch outside the ICU has any benefit, perhaps in patients in whom the endothelial glycocalyx is better preserved (in the operating room, or in the emergency room for acute trauma patients, for example), is a question that remains to be answered.
Crystalloids can be used to achieve blood volume increase in most patients – but more volume will be required (albeit modest in septic patients) than with the use of HES. For patients in which this excess volume is undesirable, HES might offer benefits – particularly in patients with intact glycocalyx. An example of one approach that might be used regarding the use of HES 130/0.4 might be that, after initial haemodynamic stabilisation/resuscitation with perhaps a combination of colloid and crystalloid, that HES should be avoided thereafter in critically-ill patients with severe sepsis.